Rheumatoid Arthritis
Rheumatoid Arthritis (RA) is a chronic, inflammatory, autoimmune disease that is characterized by inflammation of the joints and can lead to destruction of joint and periarticular tissue. There is also a wide variety of extra-articular changes.
It is a chronic disease because it has no cure, but if effectively treated, it has a good vital and functional prognosis. In recent years, there has been a substantial improvement in the treatment of this disease. On the one hand, there has been an improvement in treatment strategies with more effective use of existing disease-modifying drugs, and on the other hand, new drugs have emerged.
RA patients often experience pain and difficulty in mobilizing the joints, but the symptoms can be very varied. Suppression of inflammation in the early stages of the disease, i.e. early treatment, can result in a substantial improvement in the long-term prognosis.
RA is not a rare disease, its prevalence (frequency) varies from 0.5-1.5% of the population in industrialized countries. In Portugal it is estimated to affect 0.8-1.5% of the population. The overall occurrence of AR is two to four times higher in women than in men. The peak incidence in women is after menopause, but people of all ages can develop the disease, including adolescents.
What's the cause?
Being an autoimmune disease means that in the patient with RA his immune system is not functioning properly and there are products of the immune system that react against the patient's tissues.
The cause of this deregulation of the immune system that occurs in the RA is unknown, however, research is being done in this area and some risk factors have already been discovered, such as smoking. Scientific studies also suggest that the disease is caused by the interaction of risk factors with the existence of genetic predisposition.
Joint inflammation is thus triggered by the presence of molecules (cytokines) that interact with some white blood cells causing a local and systemic inflammatory reaction (throughout the body). This process translates into edema (swelling), pain, and sometimes redness (redness) and an increase in temperature in the affected joints, causing inability to move them properly.
What complaints and symptoms do patients have?
The presentation can be very variable. The presence of arthritis (inflammation in the joints) is a fundamental characteristic of the disease. Joint inflammation causes characteristic changes: oedema, joint pain, and sometimes redness and heat. It also causes stiffness, a sensation of prison of movements, especially in the early morning or after periods of rest.
Often the disease starts as a symmetrical polyarthritis (more than 4 swollen and painful joints on both sides of the body). Any joint with a synovial membrane (membrane that coats some joints and produces a liquid that lubricates, nourishes and facilitates joint movements) can be affected, but usually affects the small joints of the hands and feet first. As the disease progresses, more joints may ignite, including shoulders, elbows, hips and knees.
In addition to joint symptoms, constitutional symptoms (e.g., tiredness, flu symptoms, fever, sweating, and weight loss) are common.
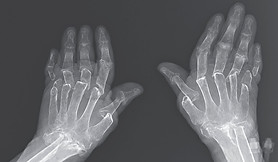
If left untreated, inflammation leads to progressive joint destruction and loss of function. Joint deformities, some of which are very characteristic of the hands, may appear at this time. To the joint damage, loss of muscle mass can be added by atrophy, which can progressively lead to motor difficulties.
The tendons are surrounded by sheaths and these are also made up of synovial membranes and can become inflamed, just like the joints.
Objectives of a rehabilitation program:
-
Improvement of joint movement and manual dexterity
-
Pain and inflammation relief
-
General physical reconditioning
-
Teaching and counseling of support products (orthoses, splints, etc.)
-
Return to work activities , daily life and sports activities
Ask our Flyers for your Hometraining at the doctor's appointment



.png)